It starts with blurred vision, sensitivity to light, and frequent changes to your eyeglass prescription, and progresses to vision loss. Keratoconus is a disease that affects more than 1 in 2,000 people in the United States, with symptoms usually starting in adolescence and progressing over a decade. If left untreated, keratoconus will steadily degrade your vision, and about 20 percent of people dealing with the disease will ultimately need a corneal transplant.
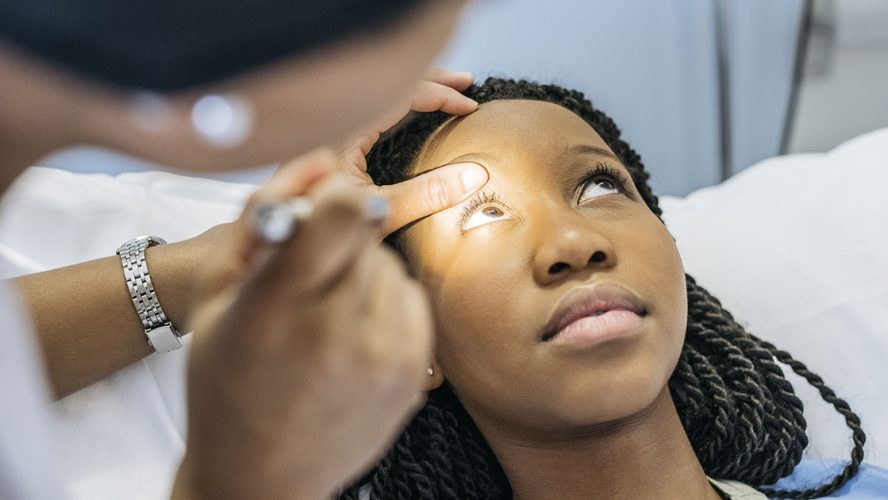
“In people with keratoconus, the normally transparent, dome-shaped cornea develops a thin, weakened area, which protrudes forward to take on a cone-like shape,” says Thomas W. Burns, president and CEO of Glaukos, an ophthalmic medical technology company. “This abnormal shape causes distortion of vision, which worsens as the cone-shape becomes more pronounced. In more than 90 percent of cases, both eyes are affected.”
A specialist
No one knows what causes the condition, which affects both genders equally and is found in all ethnic groups. In the early stages of keratoconus, updated prescriptions for glasses or contact lenses can improve vision, but it is a progressive condition; once keratoconus is diagnosed, it’s only a matter of time before glasses and contact lenses will become ineffective.
“Up until we had collagen cross-linking,” says Dr. Brandon Ayres, a board-certified ophthalmologist at Wills Eye Hospital in Philadelphia, “there was really nothing we could do with keratoconus as far as real intervention. It was just basically watch, follow, and do surgery when necessary.”
Treatment
Corneal cross-linking, like the iLink procedure from Glaukos (the only FDA-approved cross-linking procedure in the United States) is one of a short list of effective keratoconus treatments.
“In collagen cross-linking riboflavin (vitamin B2) is absorbed by the cornea, and then the eye is exposed to calibrated ultraviolet light,” explains Dr. Ayres. “The interaction between the collagen fibers, the riboflavin, UV light, and oxygen biomechanically strengthens the cornea.” The results have given hope to keratoconus patients everywhere. “In the FDA studies, cross-linking was shown to stop progressive keratoconus in 95 percent of patients,” notes Dr. Ayres. “In many cases, you actually will see a little bit of regression.”
Cross-linking procedures have changed the “paradigm of treatment” and offer hope to young people whose vision is threatened by the disease. “The goal now is to catch these patients very early before they progress to end-stage care,” says Dr. Ayres, “so they never need a corneal transplant.”