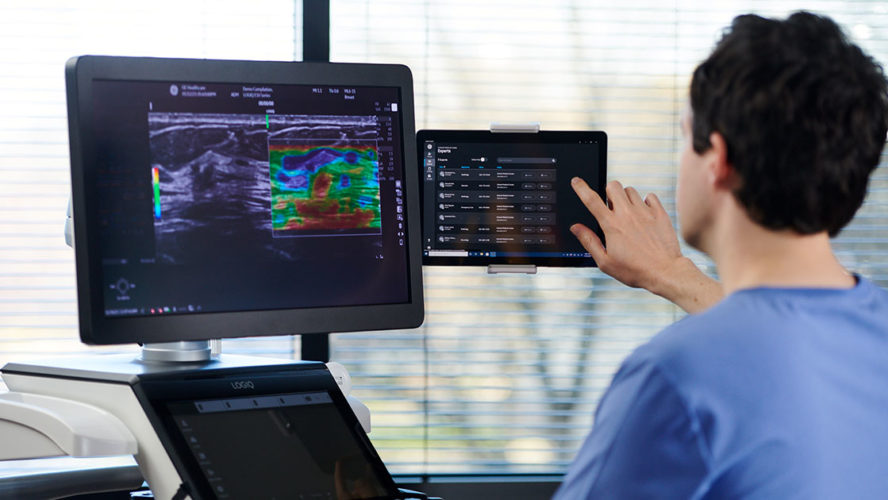
Radiologists and sonographers suffer from high levels of burnout. The solution might just be better technology.
Most people don’t think of radiology or sonography as high-stress careers, but the statistics tell a different story. More than 60% of radiologists report suffering from burnout[1], according to the National Institutes of Health, citing overwork and feeling underappreciated. And a study from King’s College London found that more than 70% of surveyed sonographers were considering leaving the profession due to workplace stress[2].
Meanwhile, the demand for radiology and ultrasound procedures is growing rapidly. The benefits of early diagnosis combined with the rise in chronic diseases and a need for less-invasive diagnostic procedures is boosting the radiology and ultrasound system market. For example, the Bureau of Labor Statistics predicts employment of medical sonographers to grow 10% in the next decade[3], adding nearly 15,000 jobs a year, aided by record-low unemployment. But in the short term, that extra demand translates to more images to interpret, more data to input — and more stress.
Challenges to well-being
With demand for radiologic scans and ultrasound exams soaring, challenges to the well-being and mental health of the experts delivering these services is mounting:
- There is wasted time and inefficiency — for example, an analysis at a Canadian hospital showed radiologists spent about 10% of their work day communicating routine results[4], while sonographers in a US hospital spent only 39% of their day on scanning activities — and up to 5 hours per day on non-scanning activities[5].
- Increasing exam complexity combined with inter-operator variability can have a negative impact on workflows, leading to frustration and lowered confidence[6].
- Outdated equipment can pose a heightened risk of repetitive stress injuries (RSIs) and other health risks.[7]
- Redundant manual data entry takes up time that could be spent on more important aspects of the work — frustration with electronic medical records is frequently cited as a major cause of burnout.[8]
- The exploding volume of exams can overtax even a fully staffed service, while manual billing and quality assurance and control procedures can result in duplicated effort and disrupted work.
One other potential cause of workplace stress and burnout for radiologists and sonographers is non-standardization of both equipment and protocols. Legacy software in picture archiving and communication systems (PACS) and radiology information systems (RIS) are often left to languish with minimal upgrades from vendors, and there can be wide variation in report terminology. These disparate approaches, systems, and vocabularies contribute to a stressful work environment.
Technological solutions
There are several effective ways to combat the prevalence of workplace burnout for radiologists and sonographers. One overall change is to implement digital workflow optimization solutions. Employing artificial intelligence (AI) and other software tools may minimize steps in workflows, reduce distractions, analyze real-time volume to make workload assignments equitable, and ensure right-size staffing as volume fluctuates. These solutions may also help standardize the equipment, terminology, and protocols used by sonographers, resulting in reduced variability in exam quality and standardization of reporting for radiologists.
Artificial Intelligence may reduce burnout in other ways. GE Healthcare’s Voluson SWIFT™ * is an ultrasound system that leverages artificial intelligence to simplify the workflow, increase efficiency, and improve accuracy. The system uses Sonolyst, a suite of AI tools that can automatically identify fetal anatomy, offer AI-assisted analysis of images, and help properly align views of the fetal brain. And adding cloud-based storage to PACS and RIS platforms can improve access to images and facilitate collaboration.
For more information about the ways technology like workflow optimization solutions and AI tools will help reduce stress and burnout for radiologists and sonographers, two recent GE Healthcare Innovation Theatre events at the 2022 Radiological Society of North America offer insights and information from industry leaders: “Digital Path to Improved Ultrasound Quality, Efficiency, and Workflow” and “A Glimpse into the Digital Future of Ultrasound.”
[1] Chetlen, Alison L et al. “Addressing Burnout in Radiologists.” Academic radiology vol. 26,4 (2019): 526-533. doi:10.1016/j.acra.2018.07.001
[2] Skelton E, Harrison G, Rutherford M, Ayers S, Malamateniou C. UK obstetric sonographers’ experiences of the COVID-19 pandemic: Burnout, role satisfaction and impact on clinical practice. Ultrasound. 2022;0(0).
[3] Bureau of Labor Statistics, U.S. Department of Labor, Occupational Outlook Handbook, Diagnostic Medical Sonographers and Cardiovascular Technologists and Technicians,
at https://www.bls.gov/ooh/healthcare/diagnostic-medical-sonographers.htm (visited November 14, 2022).
[4] O’ Neill SB, Vijayasarathi A, Nicolaou S, et al. Evaluating Radiology Result Communication in the Emergency Department. Canadian Association of Radiologists Journal. 2021;72(4):846-853.
[5] Hoffman K, Evans J, Kershner P, Haurani MJ, Satiani B. Analysis of Lost Sonographer Productivity in a University Hospital Vascular Laboratory. Journal for Vascular Ultrasound. 2015;39(2):78-80.
[6] Reiner, Bruce I. “Strategies for radiology reporting and communication. Part 1: challenges and heightened expectations.” Journal of digital imaging vol. 26,4 (2013): 610-3. doi:10.1007/s10278-013-9615-6
[7] Muir, Marylou & Hrynkow, Paul & Chase, Robert & Boyce, Dianne & Mclean, Daria. (2004). The Nature, Cause, and Extent of Occupational Musculoskeletal Injuries among Sonographers. Journal of Diagnostic Medical Sonography. 20. 317-325. 10.1177/8756479304266737.
[8] Christopher R. Bailey, Allison M. Bailey, Anna Sophia McKenney, and Clifford R. Weiss “Understanding and Appreciating Burnout in Radiologists.” RadioGraphics 2022 42:5, E137-E139
*Voluson Swift is a trademark of GE Healthcare.