Shannon Hader
Deputy Executive Director, Joint United Nations Programme on HIV/AIDS (UNAIDS) and Assistant Security-General, United Nations
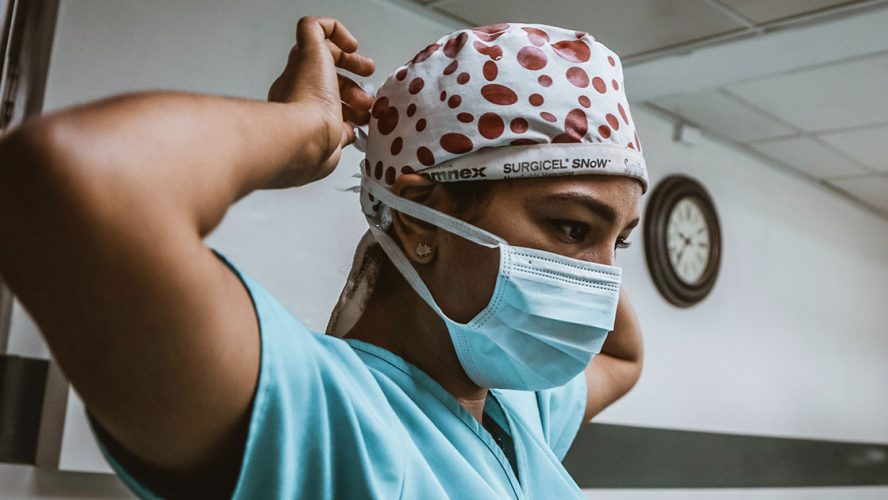
A leading HIV/AIDS expert says interruptions in treatments and services for people living with HIV during COVID-19 could have deadly consequences.
“A six-month interruption in HIV treatment just for sub-Saharan Africa would cost, just in the first year, 500,000 additional deaths,” said Shannon Hader, the deputy executive director of the Joint United Nations Programme on HIV/AIDS (UNAIDS) and assistant secretary-general of the United Nations. “That doubles the number of deaths in one year from HIV and it actually pulls us back to the 2008 death rates from HIV. We would lose over a decade of progress in just one year.”
That’s according to research modeling work UNAIDS did with the World Health Organization, the Bill and Melinda Gates Foundation, and five prominent HIV modeling research organizations.
The “bad case scenario” research model looked at sub-Saharan Africa, where so many people live with HIV.
“We think it’s totally possible to act, so we don’t think that’s going to happen,” said Dr. Hader, who guides UNAIDS’ efforts in promoting an expanded and integrated United Nations system response to HIV around the world. “But people have to realize that autopilot, it’s not going to work. The costs are real for people.”
While people with HIV are not necessarily at greater risk for contracting COVID-19, they often have comorbidities including heart disease, lung disease, or obesity, which could put them at greater risk for contracting the novel coronavirus.
She wants people living with HIV and their families to know the bad case scenario doesn’t need to happen. They can drive and demand solutions, and UNAIDS and other organizations want to support them.
Helping vulnerable populations
Dr. Hader compares COVID-19 to HIV. While they are two different viruses, COVID-19 and HIV both started out as unknown diseases. They have common lessons, especially about empowering communities to take action, fighting against stigma, and never compromising on human rights.
“It is incredibly important to make sure the vulnerable and the most marginalized are best supported during this time,” Dr. Hader said. “As we discover treatments and vaccines for COVID, we need to make sure these technologies and tools are accessible to even the most poor and marginalized, and that they’re not monopolized or hoarded, and we’re not keeping those most vulnerable last in line.”
Dr. Hader is concerned people with HIV might be further discriminated against during the pandemic, including not getting the social support they need, including food, income support, and clean water.
She encourages leaders to take a human rights-based approach to ensure vulnerable populations get the care and respect they deserve. For example, in many places around the world, people with HIV worry about treatment interruptions. They often have to get their medicines every few weeks or monthly. But now, many of them are able to get three to six months of supplies and medicines at once. That’s an important step to helping vulnerable populations.
“A lot of our attention is how to help countries, help communities, get individuals what they need to not have services interrupted,” said Dr. Hader, noting people feel more confident and in control when their needs are met.
Advocacy
She says it’s essential to set up global solidarity and transparency, and to invest in the technology and tools needed. For example, healthcare workers around the world need personal protective equipment, and people worldwide need affordable access to COVID-19 testing and treatments as they become available.
“I want everybody living with HIV to feel confident that they know the basics about COVID,” said Dr. Hader, encouraging people to be their own health advocates. “I would love for everyone living with HIV to feel empowered to take prevention measures, whether it’s hand washing, wearing masks, or physically distancing.”