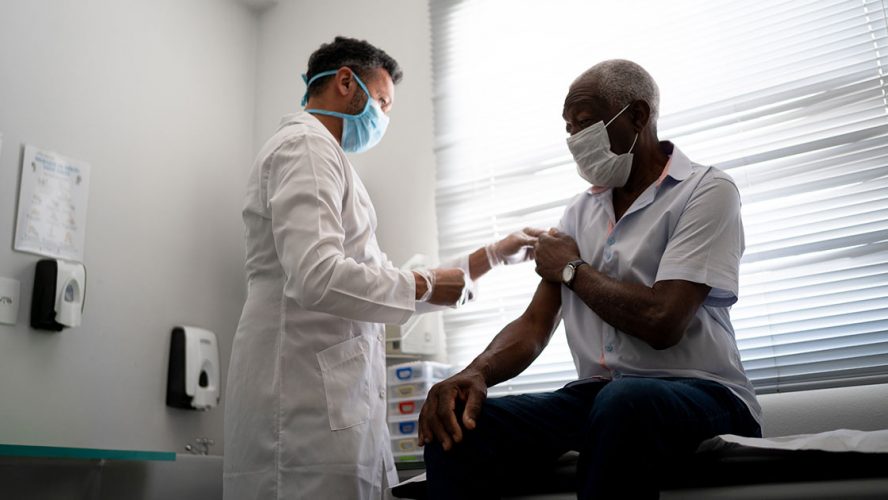
Patients with an advanced lung cancer diagnosis face many choices in their journey. One option for some patients is to enroll in a clinical trial – particularly for patients whose cancer has advanced to a stage where new treatment options are needed.
“When we talk about clinical trials to patients, we tell them it’s an opportunity to access investigational therapies while still in clinical development,” said Upal Basu Roy, PhD, MPH, Executive Director, LUNGevity Research at LUNGevity Foundation, an organization committed to accelerate research and providing community, support and education for those affected by lung cancer. “Ten years ago, I would have told you a different answer, but right now, a lot of lung cancer patients are considering clinical trials even in first line treatment.”
There are many opportunities for patients enrolling in a clinical trial. “Patients often say their biggest reason to enroll in a trial is to have access to [potentially] life-saving therapies while still being developed,” said Roy. “The second reason is for the benefit of science and helping others.”
There are over 500 lung cancer clinical trials currently open and enrolling, according to Clinicaltrials.org. The types of trials vary and are based on the line of therapy and the type of therapeutic intervention. “Some studies include a single agent treatment, or combination, and a different mode of administration, like pills or infusions,” said Dr. Roy.
Studies with infusion-based products typically include a fixed number of cycles of therapy, while studies of oral therapies require continuous therapy until the disease progresses. Some treatments, including cell therapy, are administered as a one-time treatment. Most studies require a commitment of two to five years to allow for patient follow up.
Patients with lung cancer, particularly those who have not responded or progress in their disease following treatment, may have a high symptom burden and need to know what to expect with an investigational therapy. “It is critical to explain to patients upfront how the trial is conducted,” said Dr. Roy. Cell-based therapies, for example, require more preparative work for the patient before the therapy is administered. Depending on the type of therapy administered, there may be frequent office or hospital visits as well as long-term follow up visits.
Despite the promise of cutting-edge science, patients may hesitate to enroll in a trial. Extra monitoring required, while positive clinically, may be an extra burden. Cost and time commitments are also deciding factors. Some trial sponsors cover some or all direct costs, including scans, travel and accommodations if the patient lives far away from the trial site. Hidden, intangible costs, like taking time off from work, should be considered.
“The single most deciding factor [for patients] is the doctor offering the trial,” said Dr. Roy. “If a physician offers it, the likelihood of enrolling is incredibly high.” In addition to physicians, patients may also consult advocacy groups or other patients who may have had experience with an investigational therapy.
Patient advocacy groups are an excellent resource for patients to find trials and information about trials. “We have a web-based clinical trial finder customized to lung cancer, to search by various criteria,” said Roy. While LUNGevity does not specifically recommend trials to patients, it educates patients through webinars about new treatment modalities, providing a forum for patients to hear directly from top physicians about these options. LUNGevity also runs clinical trials through its in-house research center to understand patient/caregiver experiences and access to care.
“Ask your doctor whether it’s time to consider a clinical trial,” said Dr. Roy.