As the prevalence of diabetes rises across the nation, so does the risk of developing serious complications like Diabetic Foot Syndrome, also known as DFS. People living with diabetes have a 25 percent lifetime risk of experiencing high-risk chronic wounds and 15 percent lifetime risk of experiencing foot ulcers. Despite these staggering statistics, DFS is an often overlooked and patients are rarely provided with effective preventive options.
Dr. Irina Saretzky, a practicing clinician, dermatologist and wound healing specialist at the Hospital de Clínicas of the University of Buenos Aires, breaks down some of the dangers that pose a risk to people living with diabetes, as well as the importance of quality care and treatments.
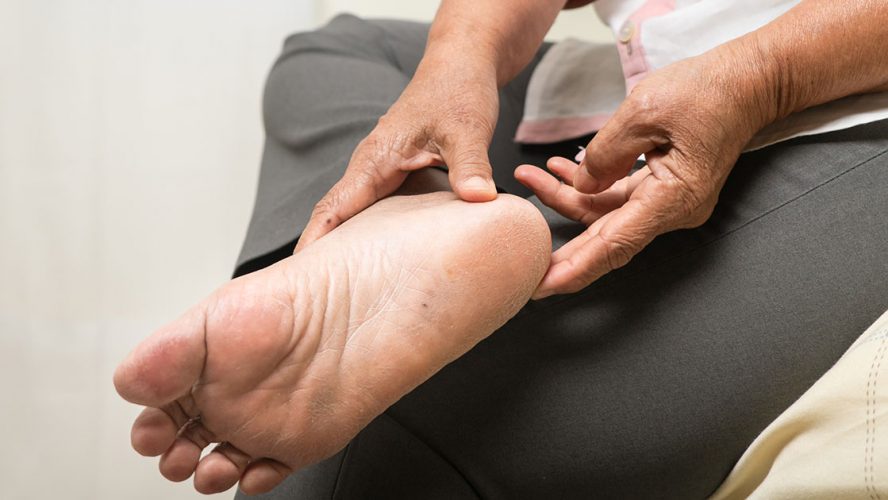
According to the doctor, most of the foot problems faced by people with diabetes arise from two main complications: nerve damage and poor circulation. Chronic nerve damage can cause dry, cracked skin, creating an entry point for bacteria and infection. Reduced blood flow in lower extremities, feet in particular, frequently cause loss of sensitivity or leg numbness, which allow small blisters to be ignored and progress to serious infections in a matter of days.
The need for a well balanced and mosturized skin
“Emollients, in particular, are crucial for skin health in patients with diabetes. Emollients provide an additional barrier of defense in the skin, preventing dry patches, reducing friction and the possibility of skin tears or cracks” says Dr Saretzky.
The skin on our feet is more delicate than we commonly believe. Heels and ankles present thinner skin, susceptible to injury from shoes, socks and stockings. While the soles of the feet present thicker skin, they tend to develop calluses or helomas due to excessive friction, weight support and dryness, making it necessary to moisturize these areas daily.
Keeping it natural
Ointments based on natural components are ideal for the care of the skin of the diabetic patient. The combination of cod liver oil, sunflower oil, and beeswax can be found in the products Dr. Saretzky is pioneering at Curefini. These natural ingredients act synergistically, improving skin barriers by preventing the water loss, cracking, and irritation that often comes with diabetic wound infections.
Curefini’s cream and ointment presentations stand out for providing a quick and effective response in protecting the skin and promoting the natural healing process, including in cases of diabetic foot.
Recommendations for General Diabetic Foot Care:
- Wash your feet every day with mild soap and warm water. First test the water temperature by hand. Do not soak your feet. Gently pat each foot dry with a towel instead of rubbing vigorously. Dry gently but thoroughly in between your toes.
- Moisturize, Moisturize, Moisturize! and use creams or ointments to keep the skin on your feet soft. This prevents cracks from dry skin and reduces the risk of infection. Focus on your heels and soles and avoid the areas between the toes.
- Elevate your legs when sitting and wiggle your toes for 5 minutes, 2 or 3 times a day. Move the ankles up and down and from side to side to improve blood circulation in the legs and feet in order to maintain good blood circulation to the feet.
- Inspect the feet every day. Look for punctures, bruises, pressure points, redness, hot spots, blisters, ulcers, scratches, cuts, and nail problems. You may not ‘feel’ that your skin has been damaged. Inspecting the skin for wounds is essential.
This article has been paid for by Curefini.
Dr. Irina Saretzky is a clinician, dermatologist and wound healing specialists currently practicing at the Hospital de Clínicas Jose de San Martin in Buenos Aires. Dr Saretzky is also a professor of Dermatology at the University of Buenos Aires, where she teaches undergraduate and graduate students, as well as a Medical Advisor to Curefini.