Terri Boyce
DNP, Member, Association of Pediatric Hematology/Oncology Nurses (APHON)
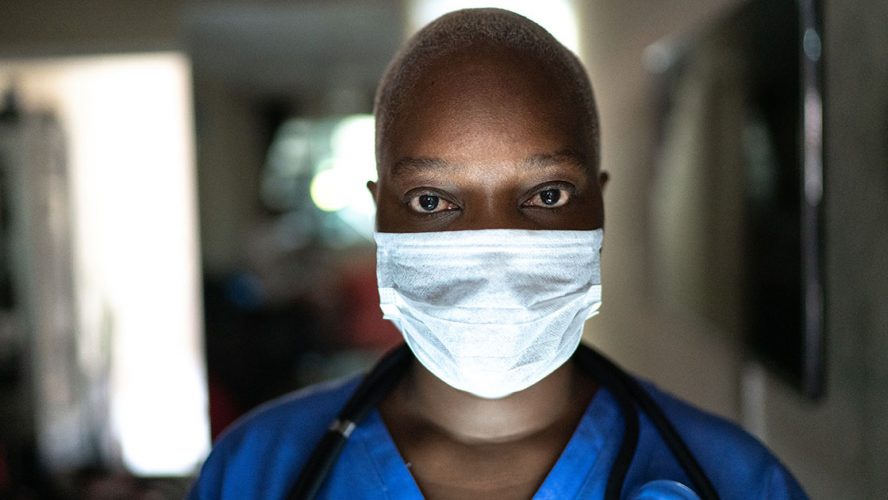
Children and adolescents with cancer experience multiple interruptions and threats to their development. Their disease and its treatment, which may last several years, can cause lifelong physical, cognitive, and psychological changes. Although most survivors are psychologically well adjusted, they experience developmental challenges related to mental health symptoms, may fail to meet expected social milestones, can experience decreased academic achievement, and find difficulty establishing employment.
Fostering resilience at all stages of disease treatment and through survivorship is an essential component of pediatric oncology nursing and leads to increased health outcomes in survivors.
The importance of connection
Resilience is the process of adequately adapting to trauma, adversity, and individual or societal tragedies while reacting positively to considerable sources of stress. Social support from family, peers, and the medical community are demonstrated protective factors for children and adolescents with cancer.
Those with increased interactions and meaningful feelings of connectedness show greater resilience and lower rates of post-traumatic stress. Finding ways to maintain these relationships is especially important while hospitalized.
Socially distanced support
The pandemic caused by COVID-19 has not only created new health concerns for this immunocompromised population, but an entirely new set of hospital policies and social guidelines which increase isolation by restricting parent, sibling, and caregiver visits to the hospital and decreasing peer interactions both at home and in the hospital.
Prior to the pandemic, children’s hospitals were filled with siblings, friends, volunteers, music and art therapists, formal and informal play therapy, and support groups. This has all now changed, and the remaining staff is creatively finding ways to persevere by engaging the patients with their family and friends at home while maintaining a safe environment in the hospital.
Internet-based video conferencing is now a regular part of our family centered rounds and technology use by even the youngest of our patients is common practice. The hospital is quieter, lonelier, and for many, scarier, than ever before, but we are all doing the best we can to maintain the cheer and hope that previously lined the hallways of the children’s cancer unit.
Thinking long-term
The long-term physical complications of COVID-19 for children with cancer are still largely unknown. However, for this already at-risk population, the impact on mental health from increased isolation and interrupted educational processes affecting their social development and overall wellbeing is of great concern for the foreseeable future. Empathy alone is not enough.
In order to provide holistic care to the family of a child with cancer, it is imperative that the bedside nurse and the multidisciplinary health care team continue to actively seek creative ways to provide patients with emotional connections with friends, family, and peers as we trudge through the pandemic and move forward into the new normal.