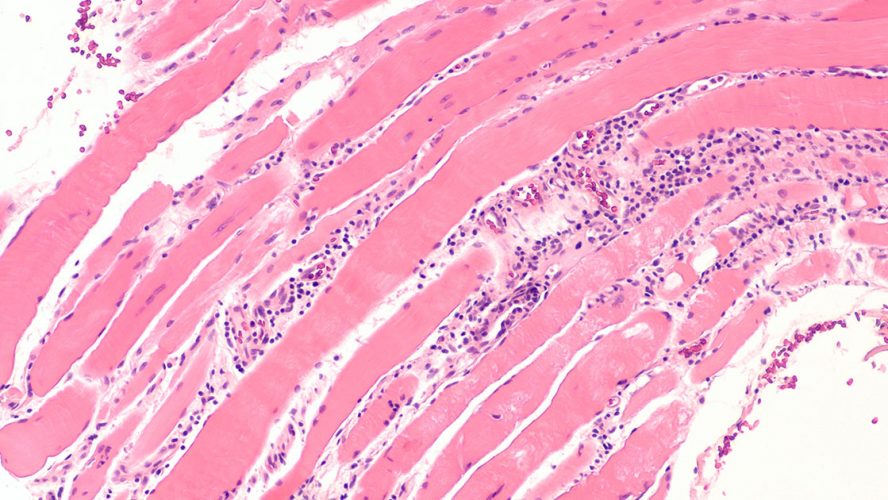
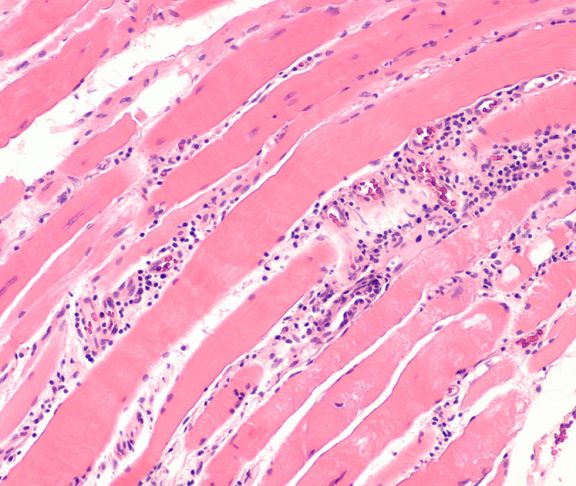
Fifty million Americans have autoimmune disease, when the body’s immune system mistakenly attacks healthy tissue. The American Autoimmune Related Diseases Association, Inc. (AARDA) says there are over 80 types of autoimmune diseases.
Inflammatory bowel diseases (IBD), like colitis and Crohn’s disease, which affect 1.4 million Americans, are autoimmune diseases. IBD patients can suffer from diarrhea, abdominal pain, gastrointestinal bleeding and extreme fatigue.
“Every patient always wants to know, ‘Where’s the next solution—the drug that’s going to cure me?’” says Dr. James Lewis, Professor of Medicine and Clinical Epidemiology at the University of Pennsylvania, who specializes in gastroenterology.
Current treatments
While autoimmune diseases aren’t curable, in many cases they can be treated. Currently doctors prescribe drugs and combinations of drugs that can reduce inflammation and manage symptoms. Still, the medicines available don’t work for everyone.
“There is definitely a portion of the population who, despite the availabilities of therapies, we can’t get to a state of remission, which is feeling like you don’t have the disease,” says Dr. Lewis, noting about a quarter of patients don’t respond to treatment.
Still he thinks there will be substantial treatment advances within the next 15 years, explaining the next step is personalizing treatments with biomarkers by finding out what types of treatments are most likely to work for a patient.
Personalized approach
Newer treatments, known as biologics are made to target specific enzymes and proteins causing inflammation. One of the latest treatments, currently in phase two clinical trials, is a precision medicine that blocks a protein called eotaxin-1, which causes inflammation in many diseases, including Crohn’s and colitis.
This new, injectable treatment is still several years away from being available, but this personalized medicine approach may offer significant relief.
“It’s the future of medicine to provide the right drugs to the right patients,” says Teper.