Dr. Jay Katz,
Practicing ophthalmologist,Director of Glaucoma Service at Wills Eye Hospital in Philadelphia and Professor of Ophthalmology, Jefferson Medical College at Thomas Jefferson University
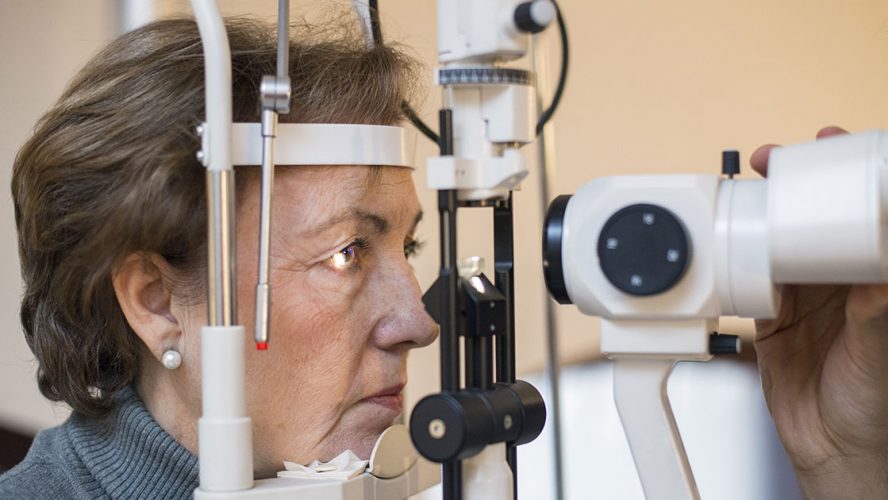
As humans age, we become susceptible to a wider range of illnesses and disorders, including glaucoma — which damages the optic nerve and is one of the leading causes of blindness in people over 60. So while we may joke about losing our eyesight as we get older, the truth is that glaucoma is no laughing matter.
Dr. Jay Katz is a practicing ophthalmologist, the Director of Glaucoma Service at Wills Eye Hospital in Philadelphia and a Professor of Ophthalmology at Jefferson Medical College at Thomas Jefferson University. Dr. Katz breaks down some of the risk factors for glaucoma, how to test for the disease, and treatment options.
According to the doctor, also the chief medical officer at Glaukos, glaucoma risk factors include elevated eye pressure, family history, a thin cornea, diabetes, low blood pressure, and sleep apnea. Near sighted and older people are also at elevated risk. A person’s race may also be a risk factor, as Black and Hispanic people seem to be more susceptible.
In order to check for glaucoma, your doctor will measure the eye pressure, examine the internal eye drainage system, and note any damage to the optic nerve by scanning pictures of tissue thickness and performing a visual field test. “These tests also determine the stage or severity of the disease,” Dr. Katz said.
Fortunately, if the glaucoma is detected, there are a variety of treatment options, including medications taken at home, in-office procedures, and surgery. “All treatments have a common goal — to lower eye pressure to an acceptable level that will halt progressive, irreversible vision loss.” You could be prescribed daily eyedrops or pills or asked to come into the office for a laser treatment. There are also a variety of surgical operations, according to Dr. Katz, such as micro-invasive glaucoma surgery (MIGS).
“MIGS operations are used often in combination with cataract surgery in glaucoma patients or alone to better control the eye pressure and reduce the glaucoma drug burden,” said Dr. Katz, referring to possible side effects of glaucoma drugs or concerns about a patient’s ability to comply with their medication regimen. The procedure involves “micro-incisional approaches” using an operating microscope to improve fluid flow patterns and lower eye pressure. Katz notes that among the procedure’s advantages are the high safety level, minimal trauma, and rapid visual recovery which allows you to quickly return to daily activities.
While the existence of effective and minimally invasive treatment options for glaucoma is great news, the even better news is that Dr. Katz anticipates even better treatment in the near future. “Rapidly evolving technologies have delivered novel, sustained drug delivery methods [such as] injectable micropolymers, tiny drug elution devices, that will decrease the burden placed on many patients who find daily eyedrop administration challenging,” he said. “[And] positive clinical experience with lasers will increase the adoption of earlier laser treatment.”
Dr. Katz also believes that as treatments continue to evolve and grow, doctors will be able to better serve their patients. “With the exciting emergence and acceptance of new approaches, both medically and surgically, physicians will be able to better tailor therapy for the best individualized care for glaucoma patients to help preserve their vision and maintain their quality of life.”