The opioid crisis has been, and remains, a unique public health challenge, and it has impacted all demographics and communities. Even though our “whole of government” approach to respond to this crisis is starting to yield results, we know there is more that can — and must — be done.
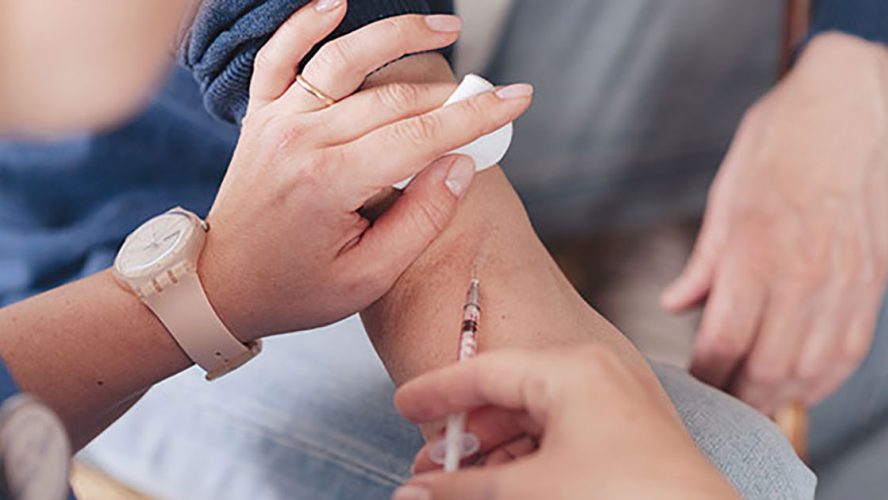
One such intervention is for clinicians to co-prescribe naloxone to patients who receive an opioid prescription, or who are considered to be at high-risk for opioid overdose. Naloxone, the opioid reversal medication, has the power to save lives, but only if it is in the right hands and administered in time.
The right Rx
In December 2018, the U.S. Department of Health and Human Services (HHS) issued guidance encouraging the co-prescribing of naloxone for patients prescribed opioids who are prescribed opioids at a dosage of 50 morphine milligram equivalents (MME) per day or higher (access CDC’s MME calculator here); have respiratory conditions such as Chronic Obstructive Pulmonary Disease or sleep apnea; are taking benzodiazepines, have a non-opioid substance-use disorder; report excessive alcohol use;or have a mental health disorder.
In addition, the HHS guidance encourages healthcare providers to prescribe naloxone to patients at high risk for experiencing an opioid overdose, including individuals using heroin, illicit synthetic opioids or misusing prescription opioids; using other illicit drugs such as stimulants like methamphetamine and cocaine; receiving treatment for opioid-use disorder, including medication-assisted treatment; and individuals with a history of opioid misuse who have been recently released from incarceration or other controlled settings.
Better equipped
Co-prescribing or prescribing naloxone to patients who meet any of these criteria can better equip patients and their loved ones to respond to an opioid overdose. For patients receiving opioids for pain treatment, it is important they understand the potency of these medications, and that they do not need to be addicted in order to experience an overdose.
Finally, the guidance also recommends that clinicians educate patients, caregivers, family membersand others who are likely to respond to an overdose on how to use naloxone, which can come in the form of a nasal spray, injection and auto-injection.
Naloxone is a critical tool to our nation’s response to the opioid crisis, and it is vital that healthcare providers talk to their patients about how it can help prevent fatal opioid overdoses.