The discovery of penicillin 94 years ago revolutionized bacterial infection treatments. However, germs adapt, and today, antimicrobial resistance is one of the most significant threats to public health worldwide.

Michael Craig
Director of Antibiotic Resistance Coordination and Strategy, Centers for Disease Control and Prevention (CDC)
Antimicrobial resistance (AMR) is a growing global health threat. AMR occurs when germs like bacteria and fungi develop the ability to defeat the drugs designed to kill them. Prior to the COVID-19 pandemic, the United States was making steady progress in reducing healthcare-associated infections, including those caused by antimicrobial-resistant germs. Those numbers reversed in 2020, partly due to inappropriate use of antibiotics and overwhelmed healthcare systems focused on battling COVID-19. Preventing infections and improving antibiotic and antifungal use are crucial to stemming the resistance tsunami we are facing.
Who’s at risk?
Antimicrobial resistance killed at least 1.27 million people worldwide and was associated with nearly 5 million deaths in 2019. In the United States alone, The Centers for Disease Control and Prevention’s 2019 Antibiotic Resistance Threats Report estimated more than 3 million antimicrobial-resistant infections occur each year, causing 48,000 deaths. During the first year of the COVID-19 pandemic, resistant infections and deaths increased by at least 15% compared to 2019.
This significant rise represents at least 29,400 lives lost from AMR commonly associated with healthcare. The overall burden of AMR in 2020 was likely much higher, as the pandemic created gaps in data collected. It is a sobering thought to know that many of these infections are preventable.
Prevention works
We know what works to fight antimicrobial resistance: preventing infections in the first place. The Centers for Disease Control and Prevention (CDC) reported in 2019 that dedicated prevention and infection control efforts drove down deaths from antimicrobial-resistant infections by 18% overall and by nearly 30% in hospitals from 2012 through 2017 in the United States.
CDC data show these reductions continued until 2020. However, the pandemic created challenges, including stress on healthcare systems, spread of more resistant infections, increased antibiotic use, and less data and prevention actions. To turn the tide, we must focus on preventing infections and improving antibiotic/anti-fungal use wherever antibiotics are used.
Simple steps
You can protect yourself, your family, and loved ones, and help slow antimicrobial resistance. A few suggested steps to reduce your risk:
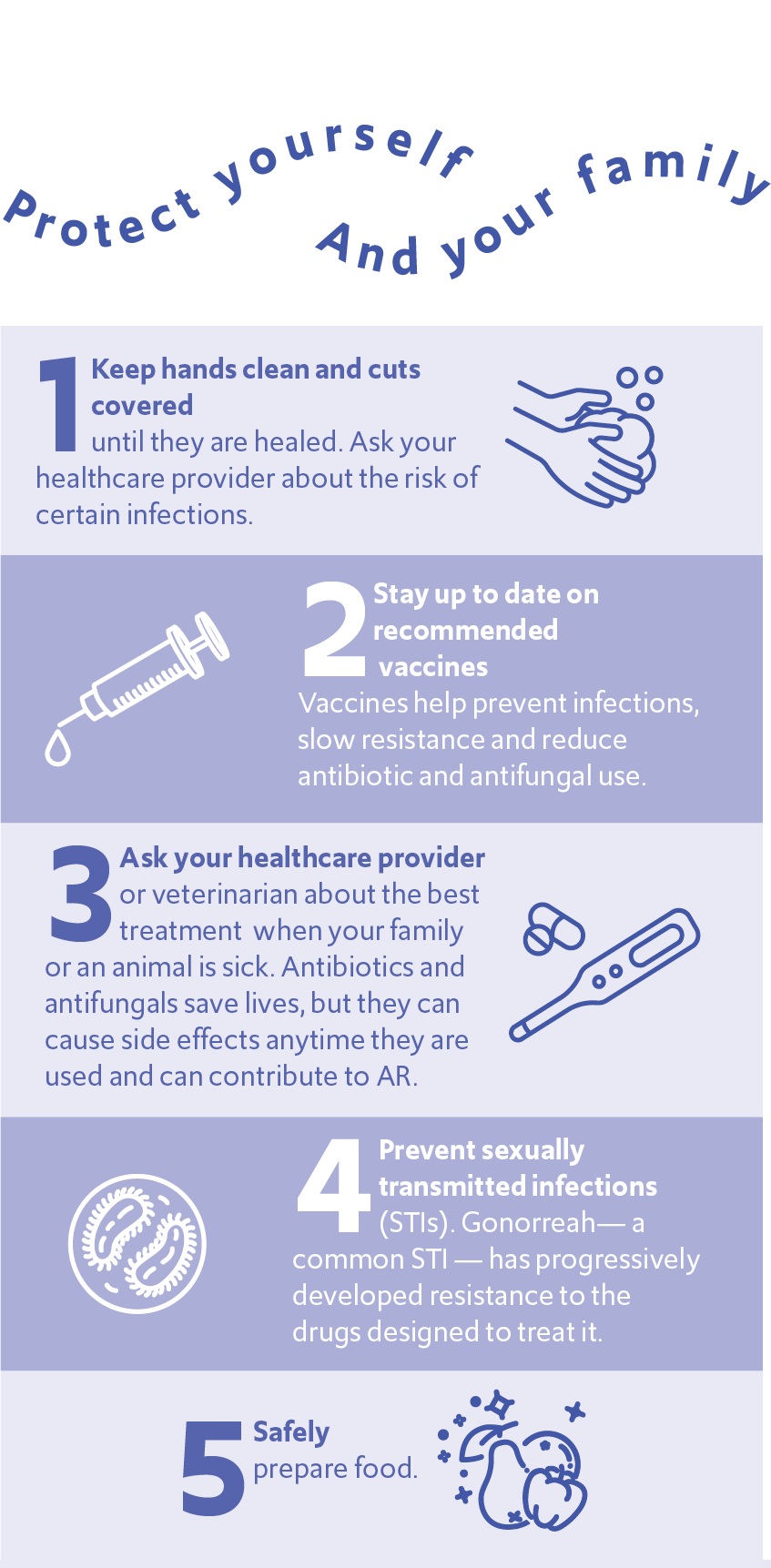
For more information, visit cdc.gov/drugresistance/protect-yourself-family.html.